BALANCE, STABILITY AND COORDINATION - THE SECRET SUPERPOWERS THAT KEEP US SAFE, STRONG AND UPRIGHT12/8/2019 Proprioception - a fancy term for a very useful sense Do you think of yourself as having good balance and coordination? Most people who rate their coordination as ‘very good' tend to be physically active, doing sports or a demanding form of dance on a regular basis. Others feel that the movement of their bodies is less than precise, like those of an awkward teenager after a sudden growth spurt. They experience difficulty calculating their height and width and constantly bump into things or often knock things over. Maybe you’ve always though of yourself as clumsy and uncoordinated, or perhaps you’re one of the many who seem to, over time, have misplaced a previously good sense of balance and now limit your activities due to a fear of falling and hurting yourself. In order for us to move in a coordinated fashion, we have to know where our body is at all times. Our proprioception makes this possible. Proprioception is our ability to feel the position of our body in space, as well as our body’s movement through space. (This ability to sense movement is also called kinesthesia, from the Greek words for movement and sensation.) Proprioception is the reason you know where your body is in space, and what position it is in, even when your eyes are closed. This system provides the necessary information for the control of posture and movement both consciously and unconsciously, and it is thanks to this amazing ability that we don’t keel over the moment the lights go out and we no longer can see our body. noun: proprioception
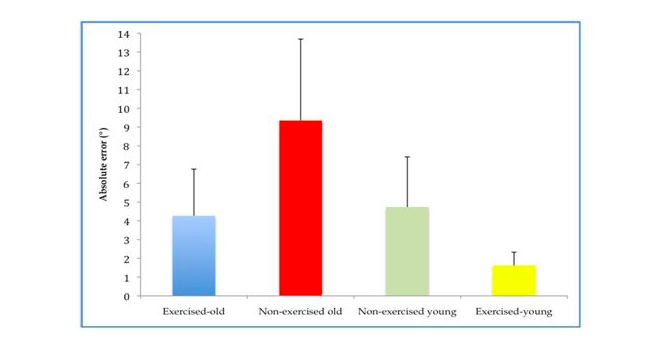
The stuff that balance is made of Mechanoreceptors are tiny, specialized sensory receptors that are located within joints, muscles (muscle spindles), ligaments (Golgi tendon organs), joint capsules and tendons. They communicate information about pressure and tissue lengthening to the central nervous system (the brain and the spinal cord), creating proprioception. The deep layers of the skin and the fascia, (the connective tissue layer that covers our muscles and organs and tie the body together as if though through a three-dimensional fishnet), also act as supplemental sources of information for our sense of proprioception. This system helps us both stand, walk and move while our conscious attention is focused on something else, and create precise movement at will. It helps us use just the right amount of muscle tension, and use our joints in a manner that is precise enough to not overload support structures such as ligaments. It helps us balance our tall bodies against the downward pull of gravity, and balance our head on our neck without unnecessary muscle tension and ligament strain. Balance is an important skill, and most commonly needed in the form of what physical therapists like to call single limb standing, ie standing on one leg. Whether you would like to walk, run, step over or into something, be it a bathtub or a pair of pants, you need to be able to balance your body on one leg. The ability to do so is a skill, and skills are composed of many components. You need the raw muscle strength of muscles such as the gluteus medius, a (as the name implies) medium-sized buttock muscle that helps keep the leg straight underneath you. You need proprioception, the understanding of what is going on based on all that information flowing to your brain and spinal cord from the mechanoreceptors throughout the body, and you need the ability to pull all that together into a movement program, created in the motor cortex in you brain. The motor cortex is where the software for our movements, or motor programs, are stored, and this software is constantly either being improved or deteriorating, depending on how much and how well you use it. When the system fails That is all fine and good, the uncoordinated and poorly balanced among us may say. Amazing as this system may be, I am still having trouble with my balance and my coordination, so what gives? This is a question with many potential answers, so let’s go through them one by one. In certain individuals one reason proprioception, and therefore balance and coordination, may be decreased, is joint hypermobility. Joint hypermobility is usually caused by a congenitally softer type of connective tissue, making joint capsules, ligaments, and tendons less resistant to stretching. A recent paper estimated the prevalence of generalized joint hypermobility in a university-aged population as 12.5%, while a more severe form of hypermobility called Ehlers-Danlos may affect as many as 1 in 5,000. Stretchier tissues will lengthen father than stiffer ones before they are triggered to signal about lengthening, and this may contribute to the decreased proprioception in hypermobile individuals. An injury, such as an ankle sprain or ACL tear, may cause hypermobility or laxity in a single joint, causing the proprioceptive input from the injured joint to decrease, leading to instability in this but not other joints. Aging tends to decrease the input from the periphery, due to deterioration of mechanoreceptors, and perhaps in part due to age-related stiffening of connective tissue, and may also change how the brain processes incoming data. Older people tend to be much less physically active than younger people, and, especially in industrialized societies, loose joint flexibility and range of motion, causing poor communication about joint position for reasons opposite of that of the hypermobile. Inactivity decreases muscle strength, but in terms of balance and stability the effect of inactivity may be even more deleterious on the levels of the “software” of the brain, resulting in a decrease in the number of brain cells dedicated to propriocetive analysis and the previously mentioned motor programs. Short- and long term dangers of poor proprioception With laxity, injuries, inactivity and aging comes a different strategy for using the body. Instead of controlling joint movements in a skilled, precise way, we start to utilize stiffening strategies, which is like moving from the smooth, controlled movements of a jumping cat to the stiffer, wobbling of a duck. This stiffening, which means we are tightening muscles as if though walking on thin, slippery ice, is neither good for muscles, which start to ache and complain under the constant burden, nor is it healthy for our joints, which are not properly protected by these inferior strategies. With decreased proprioceptive prowess, decreased muscle strength, less effective stabilizing strategies and less impressive brain software comes an increased risk of acute falls and injuries, which can be devastating and present an enormous problem among the elderly. A decreased sense of joint position and movement can also lead to less stability of and a less precise use of joints. This, in turn, can lead to microtraumas, tiny but cumulative injuries, that wear out cartilage and keep muscles and ligaments in a perpetually irritated state, ligaments because of the painful pulling on them and muscles due to the resulting chronic, compensatory stiffness. Fear not, there is great news! So are the stretchy, the injured, and the aging among us doomed, (not to speak of those that are stretchy, injured and growing older)? As always, exercise to the rescue! With continued activity and exercise that challenges and strengthens our body we can all improve, sometimes tremendously so. Due to the incredible plasticity of our body, or the ability to continuously change in order to adapt to the demands placed upon it, we can all compensate for imperfection in one organ by improving another. The initial instability caused by a torn ligament, such as the ACL or MCL ligaments of the knee, can, through therapeutic exercise, be compensated for by increasing reliance on inputs from other tissues. The incredible muscle control of a classical dancer, who typically is quite hypermobile, is a beautiful demonstration of this ability to adapt and compensate trough continuous training and effort. The negative effects of aging are as much a correlation with increasing levels of inactivity as they are a result of inevitable aging-related changes in tissue. Regular physical exercise maintains the joint position sense, or the proprioceptive ability to feel our joints, of older individuals at near that of non-exercised younger individuals and more than twice as good as that of sedentary older individuals. As a matter of fact, the only strategy that seems to retain or help regain joint proprioception in older individuals is regular physical exercise. Positive effects of regular physical exercise on knee joint position sense (adapted from Ribeiro & Oliveira, 2010) Conclusion: start where you are, seek expert advice and keep going! So whether you have fallen prey to the myth that aging inevitably incapacitates you, or have lost the ability to move without pain in joints --unstable due to inborn laxity, accidents or both-- or whether you’ve been neglecting physical activity lately, or even always, there is a right place to start and much improvement to be had! Perhaps just as importantly, exercise of the right kind can be an invaluable tool for those with enough foresight to want to prevent injuries, whether due to the fact that they are hypermobile, new to exercise or are lucky enough to be getting older. No matter what the case may be, seeking the advice of a skilled physical therapist may make the difference between success and failure. Our bodies and brains are designed to survive in the moment and will always find a way to perform a movement, no matter how. This means that we almost inevitably end up with potentially harmful compensatory movement patterns. We wobble this way and that, overuse one muscle in order to not use another weak one, and rarely, if ever, find our way back to perfect, natural movement simply by engaging in a sport, a form of exercise, or dance. How we move is just as important as the movement itself, so seek the advice of a physical therapist familiar with your situation for guidance abut how to gradually, safely and effectively find the way back to the best version of you!
6 Comments
12/15/2019 05:15:36 pm
Love this article. Full of great information. I train for SAQ, balance, grip strength, coordination, heavy circulation, proprioception. So important for hypermobility.
Reply
HypermobilityDoctor @ Lilian Holm Wellness
12/16/2019 08:51:22 am
So glad you enjoyed it! Great to hear you work on all those important skills. While we all may have a range for our function that is different from that of others, we can all aspire to be at the top of our own available range, feel the best that we can feel - now and in the future
Reply
Dexter Tamara
5/30/2022 12:34:13 pm
Reply
Jred Hatty
8/3/2022 03:42:18 pm
I TESTED POSITIVE FOR HSV-2 A FEW MONTHS AGO.
Reply
8/9/2022 11:17:58 pm
I'm glad that you talked about the importance of understanding the experience with your height and weight for proper management. I have a cousin who is an athlete that suffered an ankle injury, and he asked last night if I had any idea what would be the best treatment to do. You did a great job of explaining the important factors of physical therapy, I'll be sure to tell him that consulting a trusted balance therapy service can help provide more information about the treatment.
Reply
Jason Bennett
10/31/2022 08:50:23 pm
Omg I Finally Got Helped !! I'm so excited right now, I just have to share my testimony on this Forum.. The feeling of being loved takes away so much burden from our shoulders. I had all this but I made a big mistake when I cheated on my wife with another woman and my wife left me for over 4 months after she found out.. I was lonely, sad and devastated. Luckily I was directed to a very powerful spell caster Dr Emu who helped me cast a spell of reconciliation on our Relationship and he brought back my wife and now she loves me far more than ever.. I'm so happy with life now. Thank you so much Dr Emu, kindly Contact Dr Emu Today and get any kind of help you want.. Via Email [email protected] or Call/WhatsApp cell number +2347012841542
Reply
Your comment will be posted after it is approved.
Leave a Reply. |
Archives
February 2024
|


 RSS Feed
RSS Feed