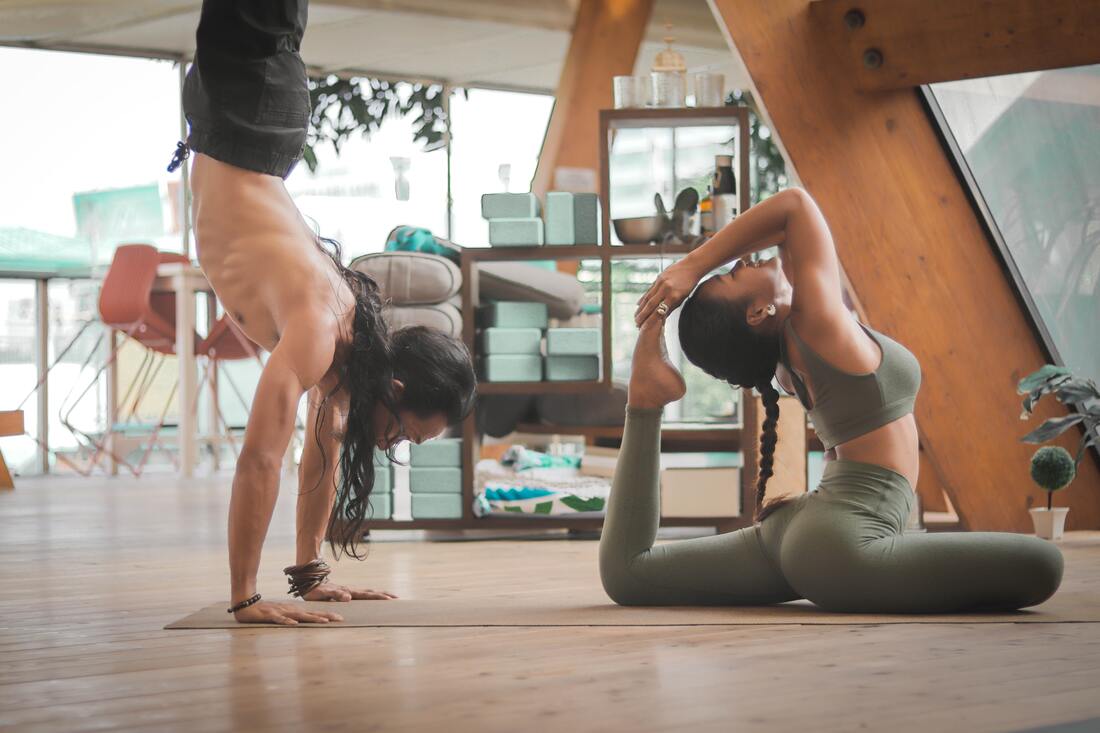 Are you, or were you once, much more flexible than most people, or do you know someone that is? The flexibility may be a sign of hypermobility, or joint hypermobility, a term that refers to joints that move beyond their normal, or average range. The current terminology for hypermobility that leads to symptoms such as pain or joint injuries is hypermobility spectrum disorder (HSD) or, if certain diagnostic criteria are met, hypermobile Ehler-Danlos Syndrome (hEDS). HSD and hEDS are, according to many experts, simply different points on a broad spectrum of hypermobility. The joint hypermobility is believed to be caused by genetic variants, (the types of which are at this point still unknown, and probably vary from person to person) in genes affecting collagen, making it less strong. Collagen is the main structural protein of connective tissue and is therefore an important component of tendons, ligaments, joint capsules, skin, bone, the fascial tissue in and around muscles and other organs etc. Connective tissue is also an important component of all the organs in the body and hypermobility therefore usually affects a variety of bodily functions in addition to its effects on the musculoskeletal system. While the hypermobility itself is more pronounced in youth, the symptoms it causes often become more apparent over time. The flexibility that once helped with dance, gymnastics or yoga may decrease, and be replaced by the joint laxity that brings on headaches and joint pain. This can lead to a downward spiral of pain and decreased physical activity. Decreased physical activity leads to weakness and further loss of stability, leaving the hypermobile joints unprotected and at risk for both acute and gradually progressing injuries. The way out of this downward spiral is correcting the weakness and lack of stability while progressively and safely increasing the amount of physical activity, utilizing principles based on an understanding of the unique needs of the hypermobile body. Basic principles for physical therapy for the hypermobile body Since in joint hypermobility, HSD and/or hEDS, joint structures such as joint capsules, ligaments and tendons acting on the joint tend to possess less stiffness, i.e. be looser, compensating for this looseness with appropriate muscle function is important. Raw strength may not be the best thing to focus on initially, but rather motor control, the control of your muscles by your nervous system. Stability is a key concept in rehabilitation of the hypermobile body. We want muscles to function effectively to prevent too much, or the wrong kind of, movement in the joints. The goal is, first, a trunk that is stable, controlled and possesses endurance. In other words, you want your trunk, from the pelvis to the neck, to be able to remain relatively stable -- but not stiff-- while your extremities move. When walking or running, the trunk does rotate a bit, but the bulk of the movement should happen in the lower extremity joints-- the hips, the knees, ankles and feet. When lifting something overhead, the movement should happen from the shoulders, instead of being achieved by arching the low back. Upon this stable trunk the shoulders and the hips control the movement of the arms and the legs. These joints also require a lot of stabilization, the work of certain muscles to guide the movement of the limbs in a stable and effective way, while keeping the joints in place, preventing subluxations and dislocations. Stabilization is a complex process which, depending on the amount and type of movement, is the end result of the nervous system functioning correctly and muscles possessing the requisite amount of strength and endurance. To (over)simplify this process a bit, think of your muscles as being able to provide either stability (the selective prevention of movement) or movement. There is a lot of overlap, but some muscles work primarily in a stabilizing function, while others work primarily as prime movers, creating movement. The stabilizers tend to be made up of muscle fibers, so called slow twitch fibers, that are weaker but possess great endurance, whereas the movement-producing muscles (fast twitch) possess greater strength but fatigue faster. This is why stabilizing exercises don’t tend to make you huff and puff, but are focused on controlling the body against gravity or movement. Do not, however, underestimate their power and importance! They may not always make you sweat, but they are the kind of exercise that stands between you and acute back spasms, subluxations and gradual degenerative injuries of your body. A very important additional effect of the exercise that rehabilitation includes is the stiffening and thereby strengthening of the softer ligaments and tendons.This directly and positively affects the ability of muscles to control joints and movement more effectively. Patience and gradual progress The various tissues of the human movement system all respond to exercise and strain, but they don’t develop at the same pace. Muscles grow bigger and stronger faster than your ligaments and tendons grow thicker and stronger. “Start low and go slow” is an oft’ repeated mantra that holds a lot of truth for individuals with HSD and hEDS. The softer connective tissue structures may actually make the individual a bit more susceptible to the naturally occurring delayed-onset muscle soreness that occurs after heavy exercise. The body repairs this micro-damage primarily during deep sleep, and since hypermobile individuals often have disrupted sleep, the repair process may be slower. The instability that may occur during movement may also increase post-exercise soreness. Expect to progress in a slow, methodical fashion. Take a step back whenever you notice any signs (fatigue, soreness, weakness, pain) that you may have been overly enthusiastic. You will eventually achieve your goal, but you can’t change the fact that it’s going to take a certain amount of time. Impatience is your enemy here, and “slow and steady” should be your mantra. Remember not to add resistance or speed until you have achieved stability! Physical therapy should not be reactive, but proactive and constructive While physical therapists have many tools in their toolbox to help with acute pain, the best use of physical therapy isn’t seeing a therapist for relief of acute pain (being reactive), but for the gradual correction of any deficits, imbalances and other problems that lead to pain in the first place (being proactive and constructive). The acute pain, if not addressed at its root cause, will come back, and over time worsen. Better to work on stability, balance, coordination, motor control and strength etc, in order to protect the body from both acute and gradual injuries. This way future occurrences of pain may be prevented, or at least decreased. You may also be able to safely move on to other types of movement, if basic strengthening and cardiovascular training doesn't appeal to you as a long-term strategy for keeping your body stable and healthy. Moving directly to other forms of movement, be they running or pilates or anything in between, may not, however, be such a good idea, as unprepared, our bodies tend to stick to their compensatory (incorrect, unhealthy) movement patterns instead of correcting themselves. Our bodies are survival machines, and will always use the strongest muscle at their disposal, and the easiest way of doing something, instead of using the weak or underactive muscles that should be learning to perform it. Being able to do something doesn’t necessarily mean that you are doing it in the way nature intended, and you may unknowingly be hurting yourself. Whether a dancer or a runner, you may be moving too much in your low back and not enough from your hips, or compensating with one muscle, for another, weakened one, and overloading the compensating areas. Yes, it is a bit complicated If all this sounds a bit complicated, it’s because it is. You need to have some understanding of both your unique, hypermobile body as well as the rehabilitative process and its principles. You need to be able to know where to start and how to progress, how to problem solve and how to adapt your exercise program to your unique needs and goals. In order to achieve your goals, you should ideally be working with a doctor of physical therapy (DPT) with experience with hypermobility. As is the case with all healthcare professionals, physical therapists don’t tend to receive much training in the management of hypermobility disorders during their educational process. Whether you’re looking for a medical doctor or a doctor of physical therapy, make sure that the practitioner you’ll be working with is experienced in treating bodies like yours. The good news is that hypermobility responds very well to rehabilitation. As a matter of fact, hypermobile individuals both benefit more from and need (specific) exercise more than other people, and it’s a medicine with only good side-effects!
6 Comments
Tracy Bogard (@weimkitty)
5/22/2022 11:09:55 pm
Thank you so much for giving out exercises so freely. The shoulder stabilizing exercise sequences on Instagram helped my painful neck almost immediately.
Reply
Lilian Holm
5/23/2022 09:37:37 am
That's fantastic, so glad to hear it!
Reply
Isabella Lucas
11/11/2022 02:19:26 pm
My ex-husband and I had always managed to stay friendly after our divorce in February 2017. But I always wanted to get back together with him, All it took was a visit to this spell casters website last December, because my dream was to start a new year with my husband, and live happily with him.. This spell caster requested a specific love spell for me and my husband, and I accepted it. And this powerful spell caster began to work his magic. And 48 hours after this spell caster worked for me, my husband called me back for us to be together again, and he was remorseful for all his wrong deeds. My spell is working because guess what: My “husband” is back and we are making preparations on how to go to court and withdraw our divorce papers ASAP. This is nothing short of a miracle. Thank you Dr Emu for your powerful spells. Words are not enough.
Reply
Dexter Tamara
5/30/2022 12:28:43 pm
Reply
8/3/2022 03:37:45 pm
I TESTED POSITIVE FOR HSV-2 A FEW MONTHS AGO.
Reply
Jason Bennett
10/31/2022 08:45:45 pm
Omg I Finally Got Helped !! I'm so excited right now, I just have to share my testimony on this Forum.. The feeling of being loved takes away so much burden from our shoulders. I had all this but I made a big mistake when I cheated on my wife with another woman and my wife left me for over 4 months after she found out.. I was lonely, sad and devastated. Luckily I was directed to a very powerful spell caster Dr Emu who helped me cast a spell of reconciliation on our Relationship and he brought back my wife and now she loves me far more than ever.. I'm so happy with life now. Thank you so much Dr Emu, kindly Contact Dr Emu Today and get any kind of help you want.. Via Email [email protected] or Call/WhatsApp cell number +2347012841542
Reply
Your comment will be posted after it is approved.
Leave a Reply. |
Archives
February 2024
|
 RSS Feed
RSS Feed